Losing My Dog, Teddy

Just after I learned I might have HHT, my family and I moved from the Boston area to Atlanta. Emory University Hospital was where I had my first PAVM embolization in 1993. The projected two hour operation extended to just over four hours, but was pronounced successful, so we were pleased. The PAVM was coiled off, my oxygenation would eventually normalize and my health seemed restored.
Routinely after the procedure, I saw a pulmonologist. Eventually he told me to just contact him if I had a problem. I was pleased that my PAVM situation seemed “cured.” So, I went on my way thinking if I stay positive, all would be well. That was my mistake. Instead of being followed regularly by an HHT Center, I neglected my internal nemesis and continued to live my life, in relatively good health, for the next 18 years.
Each morning I would rise about 7 a.m. and take my dog, Teddy, for a mile or two walk. This particular morning was no different. On a slight incline, at the edge of the woods on my own property, having walked less than a quarter of a mile, I was out of breath, my heart was racing and I could barely make it back to the house. I lay on the couch for two hours thinking this new event would resolve itself. Nothing changed. Still weak, I called a friend to drive me to the emergency room.
There I was, at age 61, in the ER, with extremely elevated blood pressure and a very high heart rate. I was taken for a heart catheterization. Those results were excellent. There were no problems seen with my heart or my arteries. I was sent home, but the symptoms continued to plague me.
My primary doctor quickly changed my blood pressure medicine, but the poor instructions given to me – even though I did call to verify those instructions – led to a more significant issue. During this two week BP medicine changeover, my heart went into Arial Fibrillation (AFIB), statistically 13 years before the average female develops AFIB. When I finally got myself to a cardiologist after feeling lousy for a couple weeks, he quickly put me back on the original blood pressure medicine I’d been on before the emergency heart procedure.
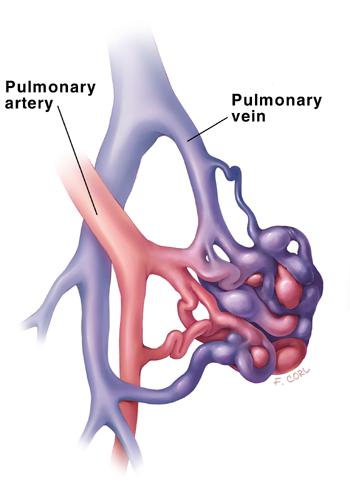
A simple PAVM with single feeding artery and single draining vein.
In my continuing attempt to feel better, I turned to a doctor specializing in asthma and allergies. He tested me multiple times, prescribed inhalers and advised me that my dog might be adding to my breathing problems. This doctor strongly urged me to give up my dog. Because Teddy and I were always in the same room and always together, it seemed to make sense that his constant presence might be adding to my asthma-like symptoms. With great sadness, I surrendered my dear, dear dog back to the rescue charity from whence he came. Happily, they found him a wonderful new home shortly after. I still inquire as to his welfare.
During my mourning period, missing my dog, many questions came to mind. Why these sudden blood pressure problems, the shortness of breath and the enormous fatigue? Why did any length walk seem so difficult for me? Could this be HHT rearing its head again? Could this be another PAVM? My primary doctor knew I had been an HHT patient with a lung PAVM. It had been in her file for nearly two decades. Why had she not picked up on this current trio of symptoms pointing directly to my lungs?
I called the HHT Center nearest me in Augusta and made an appointment for evaluation. Sure enough, I had several PAVMs which needed embolization. Now, what complicated my situation was that with AFIB, the cardiologist wanted me to be on blood thinners, but you cannot take them with active PAVMs. Therefore, with the combination of AFIB and HHT, with no remedy to keep my blood thinner, my risk of stroke is higher. I spent the next three years having multiple embolizations.
This flurry of inaccurate diagnoses; an unnecessary, high risk procedure; inappropriate prescriptive measures; and delayed remedies worsened my health and cost me my dog. I have learned to never turn my back on HHT.
